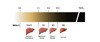
Pathogenesis of Fibrosis with Chronic HCV Infection
Hepatic fibrosis is a dynamic scarring process in which chronic inflammation stimulates production and accumulation of collagen and extracellular matrix proteins.[1,2] The hepatic stellate cells are the primary cells responsible for producing these extracellular matrix proteins. Over time, with chronic hepatitis C virus (HCV) infection, the total extracellular matrix protein content increases, and fibrosis can develop, with potential progression to cirrhosis.[3] This dynamic process can also involve remodeling and regression of the fibrous tissue via breakdown of the matrix proteins by the protease enzymes matrix metalloproteinases (MMP).[2,4]
General Approach to Evaluating Liver Fibrosis
Fibrosis is a precursor to cirrhosis, and establishing the severity of liver fibrosis helps predict liver-related morbidity and mortality, as well as to inform the need for hepatocellular carcinoma (HCC) screening in persons with chronic HCV. Noninvasive methods to estimate hepatic fibrosis are commonly used in clinical practice as a safer, more accessible, and less costly strategy than liver biopsy for stratifying persons according to risk.[5,6,7] These methods include indirect biomarkers, direct biomarkers, and elastography.[7,8,9] If a combination of noninvasive methods provides a clear-cut assessment of hepatic fibrosis, further assessment with liver biopsy is generally not needed.[10,11] Although liver biopsy with histologic analysis has long been considered the gold standard evaluation of hepatic fibrosis, it is now infrequently used for evaluation of liver fibrosis in persons with chronic HCV.[12] In the current era, the optimal approach to fibrosis assessment is to use noninvasive serum markers/tests in conjunction with transient elastography. If transient elastography is not available, two different noninvasive serum markers/tests should be used.
 Elbasvir-Grazoprevir Zepatier
Elbasvir-Grazoprevir Zepatier Glecaprevir-Pibrentasvir Mavyret
Glecaprevir-Pibrentasvir Mavyret Ledipasvir-Sofosbuvir Harvoni
Ledipasvir-Sofosbuvir Harvoni Ribavirin Copegus, Rebetol, Ribasphere
Ribavirin Copegus, Rebetol, Ribasphere Sofosbuvir Sovaldi
Sofosbuvir Sovaldi Sofosbuvir-Velpatasvir Epclusa
Sofosbuvir-Velpatasvir Epclusa Sofosbuvir-Velpatasvir-Voxilaprevir Vosevi
Sofosbuvir-Velpatasvir-Voxilaprevir Vosevi